Dual-Surgeon Spinal Deformity Surgery
Share this
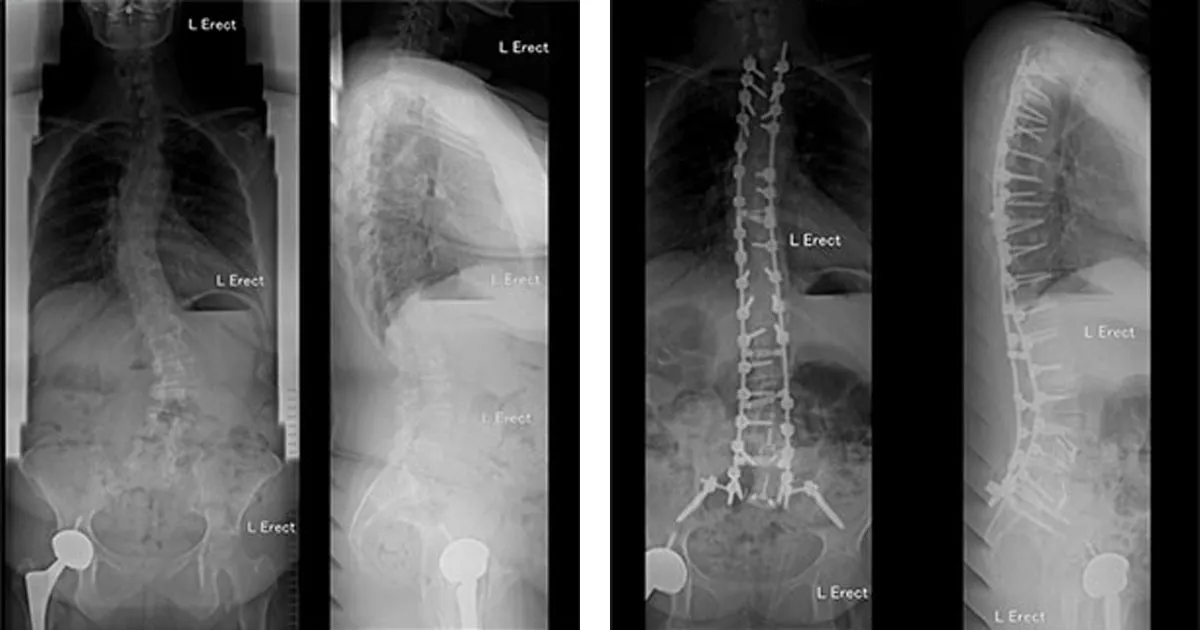
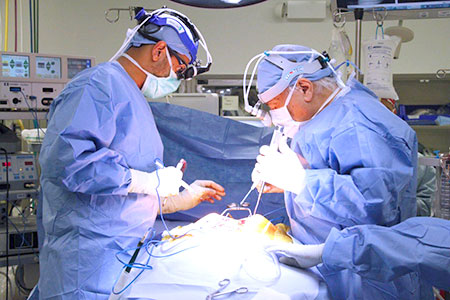
Image above: Before (L) and After (R) Dual Surgery Deformity Surgery
Even among Fellowship-trained Deformity Surgeons, many studies show intraoperative adverse events and related postoperative complications rate of 10 to 15%. Significant blood loss in posterior spinal fusion (PSF) surgery for paediatric and adult scoliosis can cause haemodynamic complications and increases the incidence of allogeneic blood transfusion. The increased risk of intra-operative bleeding is related to the long incision, extensive soft tissue dissection, multi-level decompression surgery, decortication of bony surfaces and prolonged operative time.
Allogenic blood transfusion and increased operative times have been associated with increased infection rate (Shen et al). Surgical site infections (SSI) in spinal deformity surgery carry a very high morbidity to the patient, the family, and a high cost to society. Operative time greater than 5 hours has been associated with higher rates of infection.
Table 1: Typical Surgical stages in spine deformity surgery
Stage 1
Exposure
Time taken for skin incision, dissection of subcutaneous tissue and paravertebral muscles to expose the posterior surface of the vertebrae
Stage 2
Screws insertion
Time taken to insert all the pedicle screws planned from the upper to the lowest instrumented vertebra
Stage 3
Release and decompression
Time taken for all facetectomies and osteotomies and decompression of neural elements
Stage 4
Correction
Time taken for insertion of the rods, correction of the deformity
Stage 5
Corticotomies and bone grafting
Time taken for corticotomies of the posterior vertebral laminae and transverse processes and laying morcelized local bone grafts
Stage 6
Closure
Time taken to close the fascia, subcutaneous tissue and skin
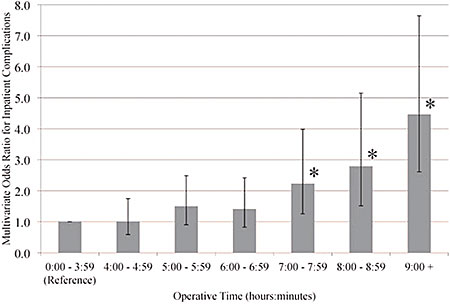
To date, many strategies have been in use to attempt to reduce perioperative complications in adult deformity surgery. These include better preoperative planning strategies, intraoperative neuromonitoring, having a blood transfusion/cell saver strategy and staging surgeries.
The utility and efficacy of 2 consultant surgeons working simultaneously has been described in the literature for procedures such as bilateral anterior cruciate ligament reconstruction, laparoscopic nephrectomy, breast surgery and esophagectomy.
Similar results were found in complex spine surgery studies. Halanski et al, Ames et al, Chan et al. reported that the involvement of two surgeons in corrective surgery for scoliosis was associated with reduced operative time, blood loss and the need for allogenic blood transfusion.
The Seattle spine team found that other complication rates were significantly lower as well when two consultant-level surgeons operated simultaneously on cases involving long fusions (16% vs. 52%). There were significantly lower return rates to the operating room during the perioperative 90-day period (0.8% vs. 12.5%), lower rates of wound infection requiring debridement (1.6% vs. 7.5%), lower rates of deep vein thrombosis/pulmonary embolism (3.2% vs. 10%), and lower rates of postoperative neurological complications (0.5% vs. 2.5%). The use of 2 surgeons experienced in spine deformity also helped achieve a decreased rate in major complications, decreased rate in premature case termination, and decreased rate of returns to the operating room within 30 days.
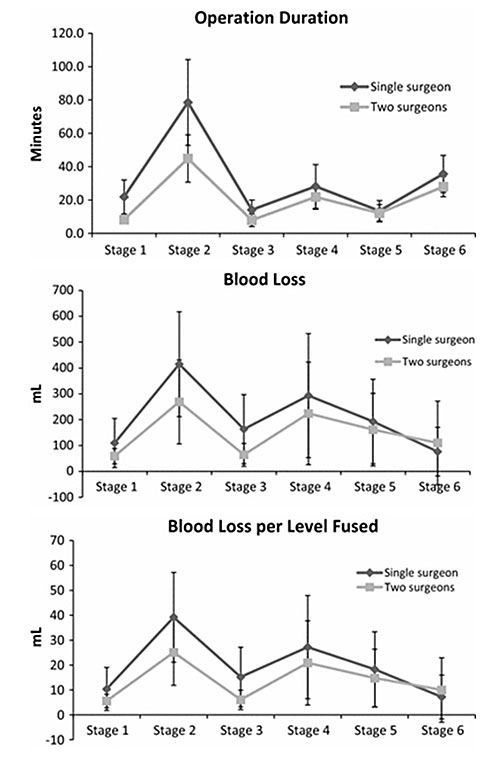
The mean operating time reported in literature for adult spinal deformity surgery involving 5 or more levels is around 300 to 360 minutes. Reducing operating time while maintaining strict adherence to good surgical technique and avoidance of intraoperative complications is key to good outcome for patients.
Since 2008, two of the authors have been performing Dual-Surgeon Deformity Surgery (DSDS) at North Shore Private Hospital. Over the last 10 years, with the additional of our third author in 2014, we have performed over 500 Dual-Surgeon procedures at North Shore Private Hospital. There has been no deep infections that required return to theatre in the DSDS group. The average surgical time is less than 4 hours and 25 minutes.
Pre-operative planning plays a major role in reducing surgical time and achieving maximum efficiency in the operating theatre. The surgical team is comprised of regular members of nursing and anaesthetic staff who are experience in all the different aspects of DSDS and are able to coordinate multiple tasks efficiently.
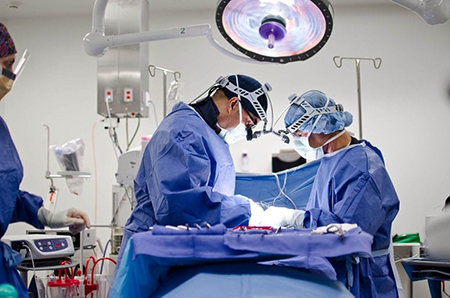
Surgery is performed in both a simultaneous and tandem manner. Each patient’s procedure is tailored to their anatomy and their needs, and different steps of the operation (such as decompression, osteotomies, correction and screw placement) are simultaneously carried out in concert. The surgical team needs to be able to cater to two surgeons performing different steps of the operation at the same time.
DSDS technique has been successful in safely minimizing overall operative time while achieving the surgical goal with a reduced infection rate.
References:
Read more
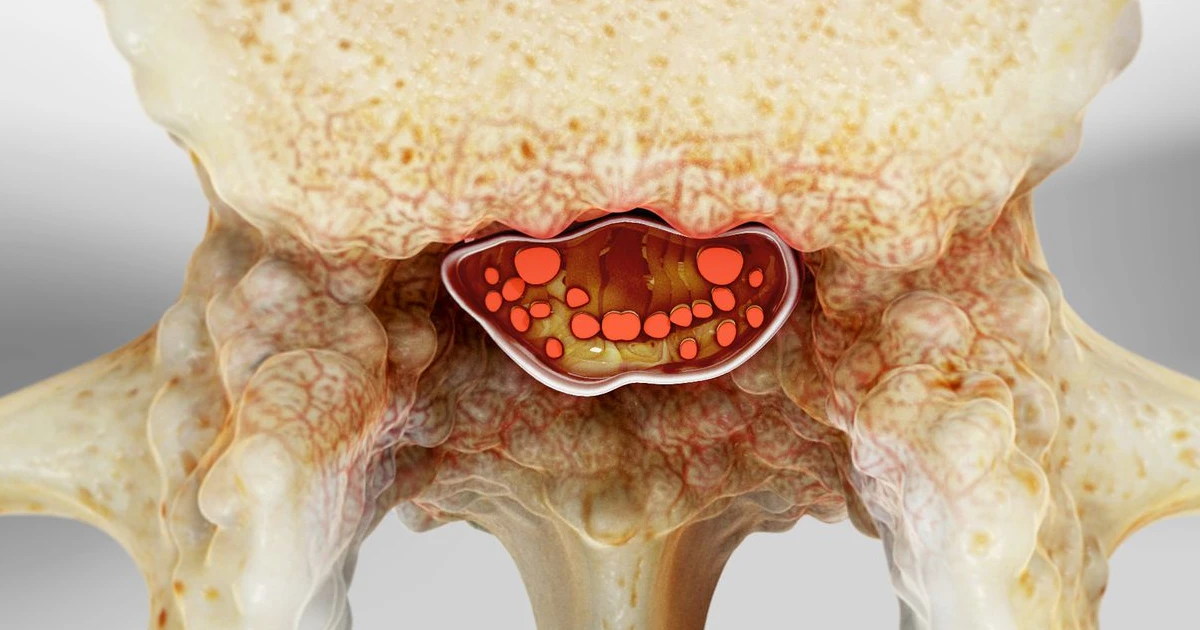
Spinal Stenosis: Understanding and Managing the Condition
Spinal stenosis refers to the narrowing of the spinal canal, the space within your vertebrae through which the spinal cord and nerves pass.
Read more

A Journey of Learning and Growth in Spine Surgery
Dr Sheng-Chieh Tseng recently completed his 2024 APSS-Medtronic Spine Fellowship report. This report reflects on an enriching three-month journey from last June to September.
Read more

Aussie teen's big dreams paused by scoliosis | A Current Affair
Dr Brian Hsu was featured on an episode of A Current Affair on 10 June 2023 on Channel 9.
Read more

International Nurses Day 2023
International Nurses Day 2023 is celebrated on 12 May. This year the theme is “Our Nurses. Our Future”. Our practice nurses are an integral part of the team and future for NSW Spine Specialists.
Read more

